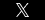Slip and fall incidents among elderly residents in nursing homes can be very serious, sometimes even deadly. One out of every three nursing home residents dies within 12 months of going to the hospital for a slip and fall. That is just an insane statistic. Our Maryland nursing home lawyers see too many nursing home fall cases with tragic outcomes. Nursing home negligence is often a major contributing factor when elderly residents fall and injure themselves. In most nursing home fall cases, the negligence involves poor facility maintenance (unkept hallways, wet floors, etc.) or negligent care by staff members (failing to put up bed rails, walking unassisted, etc.). In some cases, however, elderly residents fall because of underlying health conditions. Orthostatic hypotension (low blood pressure) is a health condition that is known to cause sudden falls among elderly nursing home residents. Nursing homes have an obligation to monitor their residents for conditions such as orthostatic hypotension and take appropriate precautions.
What is Orthostatic Hypotension?
Orthostatic hypotension (also known as postural hypotension) is a sudden drop in blood pressure that often occurs when someone gets up from a lying down or sitting position. The term “orthostatic” means an upright posture, and “hypotension” is the medical term for low blood pressure. The clinical definition of this orthostatic hypotension is when standing or sitting up causes blood pressure to drop more than 20 in systolic (top) and 10 in diastolic (bottom) pressure.
So if blood pressure is dropping from 120/80 to 100/70 after standing up, this would be considered orthostatic hypotension. When a person sits or lies down, blood collects or pools in the legs or lower body. When a person gets up from this lying down position, the collection of blood in the legs means that there is less blood available to circulate to the heart and brain. This happens in people of all ages.
In a normal, healthy person, specialized cells near the heart (baroreceptors) automatically sense this lowered blood pressure when standing up. In response, the baroreceptors are supposed to signal the person’s heart to pump faster and stabilize blood pressure. Orthostatic hypotension happens when this natural process of counteracting lowered blood pressure when standing up does not function properly. In a person with orthostatic hypotension, the baroreceptors do not trigger the appropriate response to counteract the low pressure when standing.
What Causes Orthostatic Hypotension?
Chronic orthostatic low blood pressure is a condition commonly associated with old age. However, many conditions are known to cause or contribute to orthostatic hypotension including:
- Dehydration: dehydration reduces overall blood volume, which can contribute or cause orthostatic hypotension.
- Cardiovascular Problems: a number of different heart problems can cause low blood pressure and prevent the body from responding properly when standing up.
- Endocrine Problems: certain thyroid conditions such as adrenal insufficiency and hypoglycemia can trigger orthostatic hypotension. Diabetes can also be a cause because it can impair the nerves that help regulate blood pressure.
Orthostatic Hypotension in Elderly Nursing Home Residents
Elderly people in nursing homes are at particularly high risk for orthostatic hypotension. Specialized cells near the heart and neck called baroreceptors are supposed to signal the heart to speed up in response to low blood pressure when standing up. However, as a person ages, the effectiveness of these baroreceptor cells rapidly deteriorates (in some people faster than others). As a result, when many elderly people get up from lying down, their body is not getting the proper signals to counteract the lowered blood pressure. This problem is compounded by the fact that elderly people are also more prone to have all the other conditions that are known to contribute to orthostatic hypotension (diabetes, cardiovascular problems, etc.).
Orthostatic Blood Pressure Can Cause Nursing Home Residents to Fall
It is well known that elderly people, especially elderly nursing home residents, are at very high risk for chronic orthostatic hypotension. A study published in the American Journal of Medicine in 2016 revealed that orthostatic hypotension is a major underlying cause of recurrent falls among elderly nursing home residents. The study looked at data from 844 elderly residents at 40 long-term nursing care facilities. The study found that elderly residents diagnosed with orthostatic hypotension were 3 to 4 times more likely to fall compared to residents with normal orthostatic blood pressure. Based on these results, the researchers strongly urged nursing home facilities to recognize orthostatic hypotension as a major risk factor for recurrent falls. The study also recommended that screening and treatment for orthostatic hypotension be instituted as precautionary measures just like bed rails and other safety measures. 
Nursing Home Negligence Related to Low Blood Pressure
The study establishing the link between orthostatic blood pressure and falls among nursing home residents is significant because it arguably establishes a new standard of care for nursing homes. In light of this study, nursing home facilities need to have measures in place to identify residents with orthostatic hypotension and treat them as “high risk” fall patients. If a nursing home or elder care facility does not make any effort to screen for orthostatic hypotension, and/or take other appropriate precautionary measures to prevent falls they could be liable for negligence or malpractice.
But we did not need a study to know that the risks associated with low blood pressure can be exacerbated by poor quality care. Low blood pressure, or hypotension, can be a serious health issue for older adults, especially if it is not managed properly. When nursing homes fail to provide adequate care to residents with low blood pressure, they may be held liable for nursing home negligence.
Nursing home negligence related to low blood pressure can take many forms, including failing to monitor a resident’s blood pressure, failing to provide medication as prescribed, or failing to respond to a resident’s symptoms of low blood pressure. Negligence can also occur when nursing home staff fail to prevent falls, which can be a common consequence of low blood pressure. In severe cases, neglecting to manage low blood pressure can result in hospitalization or even death.
To prevent nursing home negligence related to low blood pressure, it is essential for nursing homes to have protocols in place to monitor and manage the condition. Nursing home staff should be trained to recognize the signs and symptoms of low blood pressure and to respond appropriately. They should also be knowledgeable about the medications used to manage low blood pressure and the potential side effects of those medications. In addition, nursing homes should provide appropriate assistive devices to help residents prevent falls.
Low Blood Pressure-related Negligence Verdicts and Settlements
YEAR / STATE
CASE / INJURY SUMMARY
RESULT
2011 – Pennsylvania
A woman returned home after undergoing dialysis. She fell outside her home after exiting the medical transport sedan. The woman suffered ankle and left leg fractures. She underwent a below-the-knee amputation and remained hospitalized for three months. The woman received a prosthetic leg and was now wheelchair-bound. She alleged that the medical transport company staff’s failure to properly assist her with exiting the vehicle caused her permanent injuries. The woman claimed they failed to consider that her pre-existing orthostatic hypotension made her a fall risk. The defense denied liability by disputing whether the fall directly caused her injuries. Following two mediations, the parties agreed to a $2,800,000 settlement.
$2,800,000 – Settlement
Contact Our Nursing Home Negligence Lawyers
If your loved one fell and was seriously injured at a nursing home facility, you may be entitled to financial compensation. Contact the Maryland nursing home negligence lawyers at Miller & Zois at 800-553-8082 for a free consultation.
 Maryland Medical Malpractice Attorney Blog
Maryland Medical Malpractice Attorney Blog